High Tibial And Distal Femoral Osteotomy
WHAT IS AN OSTEOTOMY?
An osteotomy is a surgical procedure where a cut is made in a bone to allow a surgeon to change the alignment. The bone is then held in its new position to allow it to heal.
Osteotomy around the knee is either performed to the femur (thigh bone) or tibia (shin bone) at the end near the knee. Sometimes an osteotomy of both bones is performed.
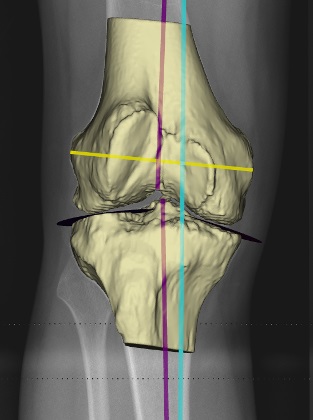
WHEN is knee osteotomy PERFORMED?
An osteotomy can be used to correct the alignment that your leg has developed. It can also be used alongside ligament surgery if you have an unstable knee that gives way.
Patients often present reporting the following:
- Knee pain in one area
- Knee swelling
- Appearance of ‘bow legs’ or ‘knock knees’.
WHAT ARE THE TREATMENT OPTIONS?
Treatment options depend on a number of factors listed in the next section.
NON-SURGICAL TREATMENT
Most people will find their symptoms improve with a good rehabilitation programme. If your knee is causing pain and this is limiting you from doing your work and/or normal activities, bracing or surgery may be an option.
KNEE BRACING AND ORTHOTICS
If your pain is due to the fact that an area of the knee is overloaded due to your alignment, specific knee braces can help offload the painful area. Most modern braces are lightweight and low profile and can be worn under clothes.
SURGICAL TREATMENT
The aim of surgery is to adjust the alignment of the leg so that the weight passes through an area of less wear and offloads the worn area. The aim of this is to restore function and relieve symptoms.
HOW DO I KNOW IF OSTEOTOMY MAY WORK FOR ME?
You will be asked specific questions about your symptoms, work, leisure activities and past medical history. You will also be asked if you smoke, as this increases the risk of infection and healing problems. A physical examination will also be required. X-rays are helpful to assess the degree of degenerative changes within the knee and specialist x-rays of the whole leg will be needed to assess the alignment.
An MRI scan can be helpful to assess the degree of wear within the knee and to assess if this is widespread or isolated.
If after this an osteotomy is a treatment option, a specialist CT scan will be performed to allow for accurate virtual 3D planning and patient-specific instruments and implants to be developed.

HOW TO DECIDE ON TREATMENT?
Factors to take into account are:
- The location of your pain
- The duration of symptoms
- If there are associated ligament injuries
- Other medical conditions
- Current lifestyle/activities
- Smoking status
- Expectations
HOW IS THE PROCEDURE PLANNED?
Mr Webb uses a surgical system that allows for the realignment procedure to be planned and performed virtually using virtual reality software. Adjustments are made to a patient specific virtual 3D model and once the optimal position is determined, bespoke surgical instruments and implants are made. This process normally takes approximately 6 weeks.
What You Want To Know About Our Osteotomy Surgery
What does Osteotomy Surgery involve?
An osteotomy surgery is performed as an inpatient procedure and requires one to two nights in hospital. This is due to the swelling and pain that is experienced and is important to monitor. A cut is made through the skin at the level of the osteotomy. The preoperative plan is then performed, with multiple checks using x-rays in the operating theatre to ensure accuracy. The procedure takes approximately two hours in most cases.
What happens before Surgery?
CONSENT:
It is important that you understand the potential risks of surgery as well as the benefits. You will have the opportunity to go through these with Mr Webb. Prior to the procedure, an electronic consent form will be sent to you that goes through the risks in detail. Please do not hesitate to arrange an appointment to discuss any questions you have.
PREHABILITATION:
Mr Webb advises that you start a physiotherapy programme prior to surgery to optimise your knee function.
The aims of prehabilitation are:
- Improve range of movement
- Muscle strength and control
- Practice using crutches
What happens on the day of Surgery?
You will be asked to come to hospital where one of the nursing staff will prepare you for the procedure. The anaesthetist will meet you to discuss the type of anaesthetic and pain relief plan for after. Mr Webb will confirm the details of the procedure with you, answer any last-minute questions and draw an arrow on your leg.
The procedure normally takes approximately 2 hours. Once you have recovered from the anaesthetic, you go to the ward. You will need to elevate your leg and use ice on the knee to reduce the swelling.
Mobility
You will require crutches for approximately 6 weeks and sometimes will be placed in a knee brace to protect the knee.
Week 0 – 4 — You will use crutches and you will be allowed to put 50% of your body weight through the operated leg.
Week 4 – 6 — You will now start to put your full weight through the leg and wean off the
crutches as guided by your therapist.
What are the risks of Surgery?
It is important to discuss the risks to ensure that you can assess whether surgery is right for you. The specific risks for meniscal surgery include:
- INFECTION — this risk of infection is less than 1 in 200 cases. Antibiotics are routinely used and are given at the start of the anaesthetic.
- BLOOD CLOTS — the risk of developing a blood clot is approximately 1 in 100. Clots in the leg (Deep Vein Thrombosis/DVT) can travel to the lung (Pulmonary Embolus/PE). Blood-thinning medication will be prescribed to try to reduce this risk.
- PAIN — most people can experience pain following surgery.
- STIFFNESS — it is important to follow a rehabilitation programme.
- BONE HEALING — an osteotomy, although controlled and accurate, is still a break to a bone. Therefore in some cases, the bone takes longer to heal and in others does not heal. This may require further surgery.
- NERVE / BLOOD VESSELS — there are large blood vessels and nerves that run close to where the operation is performed. The risk of injury to these is reduced using patient specific guides.
- COMPARTMENT SYNDROME — this is when swelling occurs within compartments of the leg. If this occurs, further surgery may be required to release the pressure within the compartments.
What happens after Surgery?
It is normal to have pain and swelling following an ACL procedure. There are cold therapy machines available to help reduce the swelling. It is a good idea to see your physiotherapist within the first week following your operation. You should use ice/cold therapy and keep the leg elevated when you are resting.
At approximately two weeks, Mr Webb will see you to review the incisions and go through the details of what was found and what was performed.
You are likely to require crutches for 2 to 6 weeks and sometimes a brace may be used to protect the knee. Depending on the specifics of the operation, your physiotherapist will start you on a rehabilitation programme that is tailored to you. Most patients will look to return to sport specific rehabilitation from 6 to 9 months, with return to play at around 12 months. It is important that this is determined by your physiotherapist.
There are cold therapy machines available to help reduce the swelling. It is a good idea to see your physiotherapist within the first week following your operation. As mentioned above, one of the risks of the procedure is nerve injury. It is normal to have some numbness and this usually improves within the first couple of weeks. At approximately two weeks, you will be seen by Mr Webb to review the incisions and go through the details of what was found and performed.
Dressings and Wound Care
You can remove the bandage after 24 hours. The sticky dressings should remain on until the two-week review even if blood stained. If they do come off they can replaced by any simple waterproof dressing.
If the waterproof dressings are intact you can shower, but do not soak the dressings and be careful not to slip or put too much weight through the operated leg. Remember, you can only put 50% of your weight through the operated leg within the first four weeks.
After your two week review, you can have a bath or swim.
Discover the Truth about Knee, Femoral, and High Tibial Osteotomy
People often have reservations about Knee osteotomy, but understanding the procedure can alleviate doubts. Osteotomy is a surgical technique that involves reshaping or realigning the bones. It is performed to relieve pain and improve function in cases of damage or degeneration, such as early-stage osteoarthritis. During the procedure, a small section of bone is removed from the tibia or femur to change the knee joint alignment, redistributing weight-bearing forces and reducing stress on the damaged area. Mr Mark Webb specializes in osteotomy surgery, providing accurate information to help you make informed decisions about your bone health. For unique solutions tailored to your specific needs, kindly schedule a consultation with Mr Webb.
